About ActiveCare Physical Therapy®
The Best Physical Therapists in NYC
-
Our therapists are licensed in New York State and active members in the American Physical Therapy Association. We have advanced training in joint mobilization and myofascial release techniques.
-
We are dedicated practitioners with a passion for the profession and a comprehensive, holistic approach to treatment and healing. We treat each patient as an individual and treat the whole person, with a plan of care designed to meet the patient’s set goals for health, functionality and a return to work, tasks and activities. We network with a team of physicians, chiropractors, acupuncturists and massage therapists in order to provide guidance to other modalities that may be effective in the patients’ care. We also offer superior Telehealth services for physical therapy.
-
Physical Therapist and owner Dr. Karena Wu PT, DPT, OCS is a graduate of the Program in Physical Therapy at Columbia University and is affiliated with several healthcare organizations in New York City. She is certified as a Strength and Conditioning Specialist, Kinesio Taping Practitioner and Pilates Instructor, and uses SpiderTech Taping. She is also a Certified Orthopedic Manual Therapist, Strength and Conditioning Specialist, Graston Technique Specialist and Pilates Instructor. She holds LSVT BIG, FMS and SFMA Level 1 certifications as well. Dr. Wu also specializes in vertigo and temporomandibular joint disorders.
-
ActiveCare is primarily an out-of-network facility. We accept all insurance with out-of-network benefits and file for most major insurance plans. We work with all prospective patients to create workable payment plans regardless of insurance coverage.
-
ActiveCare accepts Medicare, No-Fault and Workers’ Compensation patients depending on schedule availability.
-
ActiveCare’s administrators provide seamless and efficient concierge-style client service to all of our patients. And the whole ActiveCare team makes sure your time with us is a beneficial, productive and enjoyable experience.
Quick Links
Manual Therapy Bursitis Plantar Fascitis Meniscus Tears Labral Tears Kinesiology Taping Pilates Rehab
Visit Our Main Website:
www.ActiveCarePhysicalTherapy.com
Blog Posts Are Below:
Author Archives: admin
Cupping Workshop NYC
‘CUPPING’/MYOFASCIAL DECOMPRESSION: What can it do for you?
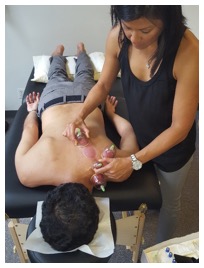
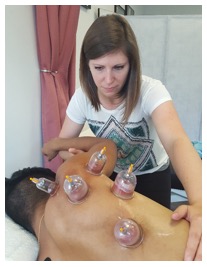
Where: ACTIVECARE PHYSICAL THERAPY, PC
12 West 37th Streetbetween 5th and 6th Avenues
Room 1202
New York, NY 10018
(212) 777-4374
When: Tuesday, August 23rd, 2016
Time: 2:00-2:30pm
You’ve seen those red spots on Olympic athletes like Michael Phelps. Many are now asking what is this new technique and what can it do for you? By now you’ve probably learned it’s called ‘cupping’ (in the medical world we call it myofascial decompression). Learn what conditions benefit from this non-invasive therapy, how quickly it works and how easy it is to get. Dr. Karena Wu and Dr. Rebecca Young will discuss and demonstrate the hottest rage in physical therapy. To register for a seat, please call us at 212-777-4374 or email us at staff@bestptnyc.com. Seats are limited.
Olympic Style ‘Cupping’ procedure in NYC
Bear The Mark of the Cup: Cupping by Best PT Karena Wu and the Staff at ActiveCare PT
ActiveCare PT in Manhattan, NY performs cupping procedures. Call today to inquire!
Karena Wu featured on Fox News: How to stay healthy during your next airport visit.
Jul. 04, 2016 – 2:53 – Dr. Karena Wu shares tips to avoid illness amid summer travel crowds on ‘Happening Now’
Physical Therapy for Knee Pain
Physical Therapy for Pain in the Knee
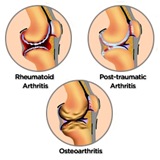 Almost every individual will suffer through some degree of knee pain throughout their lives, with chronic arthritis of the knee the single largest cause of chronic disability in Americans older than 65. Whether caused by arthritis, overuse of the muscles, a sprain or strain of the knee, or foot pronation while running (an inwards curl of the foot during movement that can result in improper weight balance) knee pain is something that affects every aspect of the body. There is good news regarding your knee pain: In many cases, it is entirely avoidable. Treatment of knee pain through physical therapy (PT) and exercise can be just as effective as invasive procedures, as proven by trials by Harvard Medical School and as published in the New England Journal of Medicine. Working on the muscles that support your knee with PT to strengthen and stretch them can provide a large degree of pain relief and help to lengthen their health. Our therapists are very capable of teaching preventative and maintenance techniques that can improve the strength of these muscles.
Almost every individual will suffer through some degree of knee pain throughout their lives, with chronic arthritis of the knee the single largest cause of chronic disability in Americans older than 65. Whether caused by arthritis, overuse of the muscles, a sprain or strain of the knee, or foot pronation while running (an inwards curl of the foot during movement that can result in improper weight balance) knee pain is something that affects every aspect of the body. There is good news regarding your knee pain: In many cases, it is entirely avoidable. Treatment of knee pain through physical therapy (PT) and exercise can be just as effective as invasive procedures, as proven by trials by Harvard Medical School and as published in the New England Journal of Medicine. Working on the muscles that support your knee with PT to strengthen and stretch them can provide a large degree of pain relief and help to lengthen their health. Our therapists are very capable of teaching preventative and maintenance techniques that can improve the strength of these muscles.
Treating Knee Pain with Physical Therapy
 The exercises your therapists will have you performing are gentle movements to relax the muscles of the knee joint in order to provide pain relief. PT will focus on improving the range of motion of your knee while reducing pain in order to restore function to your knee. Our therapist will also teach you how to avoid knee pain during your treatment by showing you how to quell your pain symptoms, such as with a warm compress or the use of a topical agent. Your therapist will likely ask you what your common day-to-day activities are and explain ways to perform them without placing excess strain upon your knee.
The exercises your therapists will have you performing are gentle movements to relax the muscles of the knee joint in order to provide pain relief. PT will focus on improving the range of motion of your knee while reducing pain in order to restore function to your knee. Our therapist will also teach you how to avoid knee pain during your treatment by showing you how to quell your pain symptoms, such as with a warm compress or the use of a topical agent. Your therapist will likely ask you what your common day-to-day activities are and explain ways to perform them without placing excess strain upon your knee.
Physical Therapy following Surgery
For patients who have had to undergo surgery due to a muscle tear or severe arthritic damage to the knee, PT is used as part of the recovery process. Depending on the cause of your knee pain, it may be possible to entirely avoid surgery through the use of physical therapy. Contact us today to rid yourself of problematic knee pain. 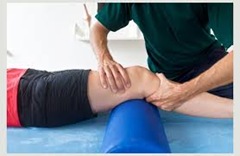
Physical Therapy for Upper Back Pain
Physical Therapy for Pain in the Upper Back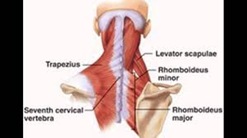
Upper back pain is becoming one of the most common sources of pain for individuals in the computer workforce, as spending a large amount of time sitting in a fixed position can place significant strain on the back. There are a number of sources of pain in the upper back, including trauma, injury, poor posture, muscle irritation, or joint dysfunction in the ribs. Our team of physicians, chiropractors, acupuncturists and massage therapists are ready and willing to work with you to help dissipate your pain and restore full movement to your spine.
Causes of Upper Back Pain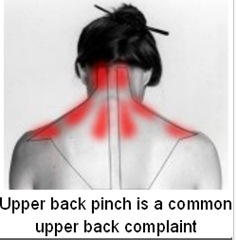
Two of the most common causes of pain in the upper back are joint dysfunction and muscular irritation. Muscular irritation commonly occurs in the muscles located across the shoulders, and is caused by either a lack of strength in these muscles or an injury due to overuse. Muscular irritation can also occur due to muscle strain or trauma.
There are two joints connecting on either side of the spine that serve as anchor points connecting the shoulder muscles to the spine. Dysfunction in these joints can cause upper back pain. Each of these causes is very responsive to physical therapy treatment,which can help to provide long-term pain relief.
Treating Upper Back Pain with Physical Therapy
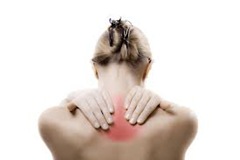 The most effective type of upper back pain treatment for muscular irritation is manual manipulation of the muscles. Techniques such as chiropractic manipulation, massage therapy, and acupuncture can each help to relax the muscles. Gentle stretching of the muscles combined with strength training can help to reduce irritation and improve the ability of the muscles to withstand use and regain function.
The most effective type of upper back pain treatment for muscular irritation is manual manipulation of the muscles. Techniques such as chiropractic manipulation, massage therapy, and acupuncture can each help to relax the muscles. Gentle stretching of the muscles combined with strength training can help to reduce irritation and improve the ability of the muscles to withstand use and regain function.
Manual treatment is also effective for symptomatic pain caused by joint dysfunction. Our therapists will help to mobilize the joints, reducing discomfort. You will also be instructed on an exercise regime to stretch the spine, shoulders, and shoulder muscles in order to successfully maintain relief. Our dedicated practitioners are trained in techniques to provide relief for the majority of upper back pain conditions.
ActiveCare PT, NYC’s best Physical Therapists Welcomes our newest PT Aide: Clare Antonioli
 A Big Welcome to our PT aide Clare Antonioli
A Big Welcome to our PT aide Clare Antonioli
Clare Antonioli is a born and bred Montanan now living in Brooklyn. She graduated from the University of Montana in 2012 with a double major in Wildlife Biology and Dance. Clare moved halfway across the U.S. to pursue her dream of becoming a professional dancer. She is currently taking classes and auditioning for contemporary companies. During her time here, Clare plans to get certification to teach Pilates. While dancing and teaching Pilates are her more immediate goals, Clare hopes to one day go back to school for Physical Therapy. In her other life, Clare is a self-proclaimed bird nerd and loves bird watching and studying ornithology. Her other passions are travel, good food, and wine. Clare is thrilled to be a member of the ActiveCare team, striving to bring the best care to our patients.
Chef Seamus Participates in the NYC Arthritis Walk, Urges Local Chefs to Join!
 Chef Seamus Mullen is a leader in raising awareness. With a diagnosis of Rheumatoid Arthritis in 2007, the publication of his cookbook, Hero Food which focuses on the healing capabilities of different foods, and his acceptance of Celebrity Honoree in the 2014 NYC Walk to Cure Arthritis, Chef Mullen has brought this disease to light for many. Interview by Karena Wu
Chef Seamus Mullen is a leader in raising awareness. With a diagnosis of Rheumatoid Arthritis in 2007, the publication of his cookbook, Hero Food which focuses on the healing capabilities of different foods, and his acceptance of Celebrity Honoree in the 2014 NYC Walk to Cure Arthritis, Chef Mullen has brought this disease to light for many. Interview by Karena Wu
Chef Seamus in the NYC Arthritis Walk
I have been a Physical Therapist for 14 years. Seamus and I were introduced by Wylie Dufresne, who is known for being proactive about taking care of his health and who was recently diagnosed with osteoarthritis himself. Seamus and I started working together in 2010 when he was trying to control the disease. Rheumatoid Arthritis (RA) is an autoimmune disease. It is a systemic arthritis where your immune system, which normally protects you against disease, mistakenly attacks your joints. RA affects 1.5 million people in the United States, if found in more women than men and commonly affects people between the ages of 30 and 60.
Chef Mullen has gone down a long and arduous path in resolving this. I am happy to share the fact that since he has altered his diet, resumed a regular workout schedule and has supplemented his health, his tests have been negative for the rheumatoid factor (RF). The RF factor is the autoantibody that is found in individuals diagnosed with rheumatoid arthritis. The higher the level of RF factor found in your system, the increased chance of articular (or joint) destructive disease.
I sat down with Seamus at his delicious restaurant Tertulia to find out more about this special Chef and his work in raising awareness for a cause dear to his heart.
What made you decide to work with the AF and when?
I was diagnosed with RA in 2007 and I soon learned that Arthritis is something that affects people of all ages! I had been so naive when it came to understanding what it meant to live with arthritis that I was pretty sure others out there didn’t know either and I wanted to do whatever I could to raise awareness and hopefully be an inspiration to others living with the disease.
What other events have you done with the AF?
I’ve done the walk, I’ve spoken on behalf of the foundation and participated in the Faces of Arthritis campaign and lots of press over the years.
What made you accept the Celebrity Honoree position?
This is a terrific honor for me, I’ve been living with RA for several years and I have gotten to a place in my life where RA doesn’t hold me back or limit me and I hope that my experience can be an inspiration to others living with arthritis understand that just because they live with arthritis it doesn’t have to derail their dreams.
How do you think this changes the walk?
Being the celebrity honoree makes the walk all that much more important!!
What has changed with you since your original diagnosis?
I went through a period of real emotional and physical distress and for quite a while it felt all-encompassing, but I’ve managed to get to a place through diet, exercise and lifestyle where I feel GREAT. This is a serious change from when I was first diagnosed.
What do you hope to inform the public about your participation?
The importance of raising awareness about arthritis as a disease that affects people of all ages. And for those of us living with Arthritis, to recognize the importance of working together, supporting one and other and ultimately not to let the disease get the upper hand! If you’re living with arthritis, there is NO need to suffer.
What do you hope to gain?
It’s always great to meet other folks in the arthritis community and broaden the outreach.
How does working with the AF impact your daily routine?
It’s great to know that there is an organization out there advocating and fundraising for the disease. I try to be as open as I can about talking about the disease and always refer folks living with arthritis to take advantage of the resources available to them through the AF.
How does it impact your work routine? Generating a team, fundraising, etc?
My team is incredibly supportive, I think last year we had one of the largest teams at the walk!!
What do you thing other chefs think about your work with the AF?
I think most chefs feel a real responsibility to their individual communities…we all like to think of our restaurants as a part of our community and working directly with charitable organizations is a big part of our roles as members of our community.
How can you recruit other chefs to participate?
Arthritis is something that effects nearly all of us…even if you may not personally live with arthritis, chances are you have a friend or family member who does and working with the AF is a great way to help those loved ones.
How can you tell chefs to do other things for social responsibility?
I think it’s pretty ingrained in the fabric of what we do. Most chefs I know are very concerned with social responsibility and contributing to their community.
What is the take home message for you and from this event?
Arthritis affects everyone!
Chef Seamus encourages his fellow chefs and industry colleagues to participate in the Walk to Cure Arthritis. The 2014 NYC walk starts in Foley Square Park and is a 3 mile (1 mile optional) walk across and back on the Brooklyn Bridge. It will be held on Saturday, May 17th. Registration starts at 8:30am and the walk begins at 10:00am. Fellow chefs and restauranteurs can form their own team to walk for a cure, or help generation donations to fund research and a cure for arthritis. Just visit www.walktocurearthritis.nyc.kintera.org.
Arthritis, In the Kitchen?
The restaurant industry is a tough business. You see the desire to get into high end restaurants, the contacts you need to get a reservation, that dreamy look when a customer has tasted something amazing and then the praise and acclaim the chef gets. ‘That was amazing! How did you do that? The flavors were incredible!’ Maybe the chef has been on TV or has a book deal in the works. You want to be that chef, don’t you? by Karena Wu
Well, those little ‘tastes’ of working in a fantastic restaurant and the celebrity status chefs get is definitely enticing. But it comes as a cost. And that cost is the long hours standing, bending forward, the intense heat and the criticism when you mess up at your station. Once you’ve gone through the school and become a chef, this is the life. You do it every day. It is normal for you and it is part of the job. You do it with a normal working body. Imagine how this might feel with a disease called Rheumatoid Arthritis?
Chef Seamus Mullen of NYC’s Tertulia and El Colmado is known as the chef with RA. Seamus became a patient of mine a few years ago. His course started in his left hip with excruciating pain and a visit to the emergency room. Multiple tests and doctor visits later, it was confirmed that he had RA. Our visits together focused on reducing his inflammation, restoring his joint immobility, reducing soft tissue restrictions while trying to maintain strength and flexibility without further irritating his already irritated joints. His biggest contributing factor: working in a hot kitchen, under stressful conditions that added more joint compression, load and irritation. Not the ideal working condition for someone with RA.
Symptoms of rheumatoid arthritis include joint stiffness, swelling and pain. The joints become inflamed during periods of exacerbation. The area gets ‘hot’, with increased skin temperature, significant swelling, and redness. The joint is ‘angry’. Typically, symmetrical distribution of joint irritation is present, meaning the same joint on both sides of the body. Also, hands are very commonly affected which means stirring, chopping, plating, all the work needed to create those magical dishes become difficult.
Other symptoms involve feelings similar to the flu: malaise, fatigue, and muscle aches. For moderate to severe RA, nodules can appear under the skin as well as the involvement of major organs like the lungs, heart and eyes.
Treatment for rheumatoid arthritis focuses on reducing inflammation and slowing or stopping the progression of the disease. Treatment includes medications, occupational or physical therapy, and regular exercise. Medications help reduce inflammation and typically work best in combination. They can include non-steroidal anti-inflammatories, steroids, biologic agents and pain killers. Physical and occupational therapy utilize manual therapies, exercises and modalities that reduce pain and inflammation and restore function. Other exercises focus on isolated joint strengthening, endurance and stability training as well as balance and proprioceptive activities. Exercises that increase flexibility and maintain strength around a joint reduce joint irritation by increasing space in the joint, reducing compression and allowing for tissue healing.
As Seamus has shown us, there are many food products that reduce inflammation. His journey in life after being diagnosed with RA lead to the creation of his book, Hero Food, which focuses on the healing power of foods. These are easily included in your diet and can make for very tasty dishes that also serve to help heal the body.
Arthritis affects the young and the old and there are many different types. This is only one type that we are discussing here. This disease did not hold Chef Seamus back. He turned his journey into a positive experience that helped him personally as well as professionally. In fact, Chef Seamus is our Celebrity Honoree at the 2014 NYC Arthritis Walk. Even with the work requirements in the kitchen, he is still able to spend time helping others with this condition. Participating in group events with a mutual cause is a wonderful way to celebrate people who have been diagnosed with a condition, but continue to live life to its fullest and keep themselves healthy and happy.
2014 5K NYC Walk to Cure Arthritis
Foley Square Park, walking across and back over the Brooklyn Bridge
5K and 3K (3 mile and 1 mile option available)
Saturday, May 17th, 2014.
Registration starts at 8:30am, walk starts at 10:00am
Physical Therapy for Neck Pain
Physical Therapy for Pain in the Neck
Neck pain can be a seriously debilitating condition, limiting your ability to perform even normal everyday tasks. Neck pain reduces the range of motion for your neck and head, and may result in pain symptoms felt in the shoulder arm or hand. Over 100 million Americans have reported having some degree of neck pain, and our dedicated practitioners understand just how serious pain in the neck can be.
Causes of Neck Pain
One of the most common causes of neck pain found in our patients is whiplash, which occurs most often from either an automobile accident or in a sports-based setting. Other causes of neck pain include complications with a cervical disc, arthritic inflammation, and as a result of poor posture over an extended period of time. Pain occurring in the neck may spread to the arms or upper back, or may result in pain felt in the head. Neck pain can also result in chronic headaches for the patient.
Treating Neck Pain with Physical Therapy
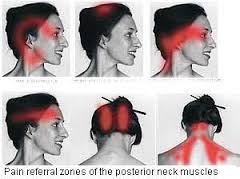
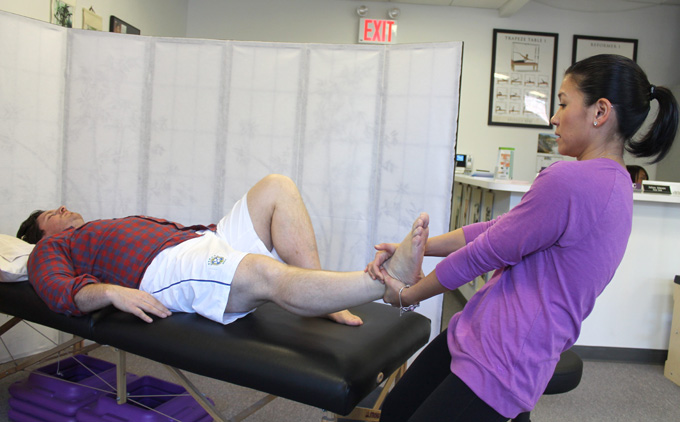
Physical therapy for neck pain focuses on both improving muscular strength and restoring the full range of motion to your neck. Stronger neck muscles will be able to better support the neck and head, reducing strain on the neck while helping to rid you of symptomatic pains. Heat, ice, and electrical muscle stimulation may also be used to provide relief to a painful neck. Our team of physicians, chiropractors, and massage therapists will device a unique treatment plan to bets help you based on what symptoms you have.
Preventing Neck Pain
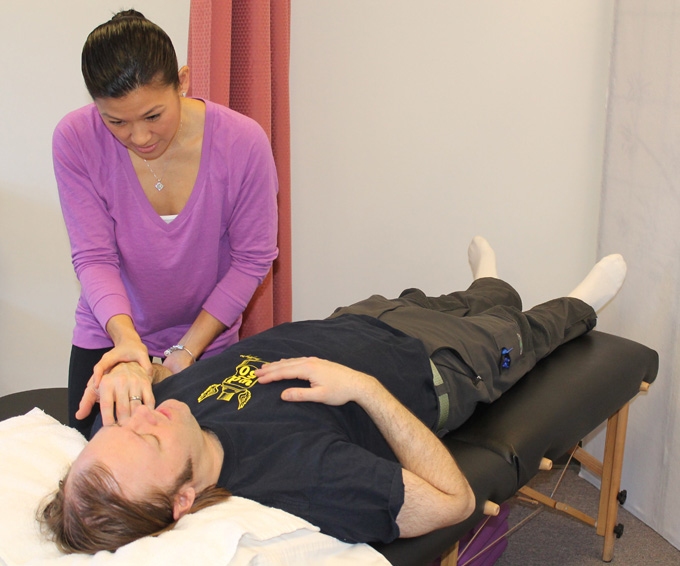
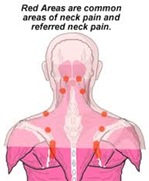 For some patients, neck pain is occurring due to causes that can sometimes be prevented. These include poor posture, sitting for extended periods of time, and having the neck twisted while resting. Our therapists will examine your posture and offer methods of posture improvement. You may also consider obtaining a cervical therapy pillow to better support your neck while sleeping.
For some patients, neck pain is occurring due to causes that can sometimes be prevented. These include poor posture, sitting for extended periods of time, and having the neck twisted while resting. Our therapists will examine your posture and offer methods of posture improvement. You may also consider obtaining a cervical therapy pillow to better support your neck while sleeping.
Physical Therapy for Thigh Pain
Physical Therapy for Pain in the Thigh
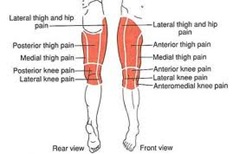 Pain in the thigh has a number of potential causes and can lead to a loss of functionality of the leg and difficulty in movement. Our dedicated team of physicians, chiropractors, and massage therapists will design a treatment based on your symptoms that will help provide relief and restore full function to your leg.
Pain in the thigh has a number of potential causes and can lead to a loss of functionality of the leg and difficulty in movement. Our dedicated team of physicians, chiropractors, and massage therapists will design a treatment based on your symptoms that will help provide relief and restore full function to your leg.
The Causes of Thigh Pain
Physical therapy is able to help with nearly every cause of pain in the thigh, studies prove. Some of the more common reasons include:
-
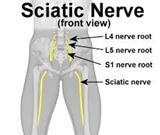
Sciatica: Leg pain resulting from sciatica is due to one or more pinched nerves in the lower back. This nerve compression can be the result of a number of spinal conditions such as a herniated or bulged disc. In addition to leg pain, you may feel weakness or numbing in your leg as well as a tingling feeling similar to pins and needles if compression worsens during movement.
-
Arthritis: arthritis comes in many forms, and can generate pain in the leg in a variety of ways.
-
Trauma: Injury to the leg is one of the most common causes of thigh pain. A pulled or torn muscle (remember the thigh contains three large muscle groups: the hamstrings, quads, and adductor muscles) can cause immense pain and affect mobility. Hamstrings in particular are at risk due to being attached to both the hip and knee joints, doubling the range of movements that can affect them.
Obtaining Relief
The exact method of restorative therapy will vary based on the root cause of your symptoms. Common methods of treatment include massage to loosen tightened lug muscles and therapeutic exercise to build strength, restore the legs range of motion, and provide pain relief. For patients with pain caused by sciatica, manual manipulation of the spine can potentially reduce the pressure exerted on the nerve to provide relief.Our experienced practitioners will create a treatment program suited to your needs.
Physical Therapy for Hip Pain
Physical Therapy for Pain in the Hip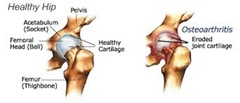
The hip is comprised of a ball and socket joint held together bynumerous ligaments, tendons, and muscles. The hips bear the vast majority of your weight during movement and are prone to arthritic pain because of it. Muscle tears or sprains may also occur in the hip if there is a sudden unexpected movement of the leg. Physical therapy (PT) is an integral factor in managing your hip pain, with your individual treatment program designed based on your symptoms.
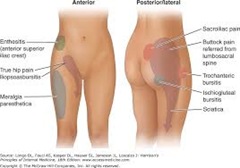 Causes of Hip Pain
Causes of Hip Pain
Depending on where your pain is and how the pain is felt, our team of dedicated practitioners will be able to diagnose the cause of your pain and help you to obtain relief. Some examples:
-
Pain in the groin, is most likely caused by arthritic inflammation in the hip joint. Muscle strains can also produce pain in this area.
-
Pain in the side of the hip is typically representative of a tear or strain in the muscles supporting the hip, with one of the more common causes being hip bursitis, which is an irritation of the bursa (a fluid filled sac between muscles and bones that allow them to move freely against one another).
-
Pain felt in the back of the hip or the buttocks is often the result of a problem in the lower back.
Treating Hip Pain with Physical Therapy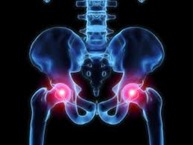
The first step in obtaining relief for your hip pain is an evaluation of your hip to examine your symptoms. We will test your walking gait, range of motion, and hip strength to help determine the cause of your pain. Our certified Strength and Conditioning Specialists will device an exercise regime based on your symptoms to help strengthen the muscles of your hip and provide pain relief. Other methods of treatment include manual manipulation of the hip to better position it while walking. For patients with arthritic pain, this manipulation will help to bear your weight more effectively, reducing the amount of inflammation in your hip.
Physical Therapy Foot Pain
Physical Therapy for Foot Pain
Physical Therapy for Foot Pain
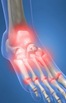 Pain in the feet can and will affect you more than you realize. Pain in the feet can adversely affect nearly every aspect of your day, and can be the source of pain felt in other areas of the body.
Pain in the feet can and will affect you more than you realize. Pain in the feet can adversely affect nearly every aspect of your day, and can be the source of pain felt in other areas of the body.
In many cases, pain of the hips, knees, lower back, and even the neck can be attributed to complications with the feet. Foot pain affects millions of Americans every year, and can occur from a minimal level of activity such as walking.
The feet create a base of support for the body, and are the starting point for many of the body’s movements. Due to the complexity of the foot and ankle (the foot alone contains 26 different bones and over 100 ligaments, tendons, and muscles), it is a common site for tears, fractures, and sprains among other injuries. Impairments in the feet that are left untreated can lead to lifelong complications and permanently reduced ability. Physical therapy (PT) is able to help provide pain relief for the feet and help patients re-achieve full usage of the feet.
Reasons for Foot Pain
Common Causes of Foot Pain
Two of the largest causes of foot pain are shoes that do not fit properly and shoes that force the foot into an unnatural shape. On average, people will take between 8-10 thousand steps each day, with each step supporting a force approximately 50% greater than their body weight. Having this 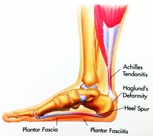 force placed directly on feet that are even slightly off-balance can result in pain or injury.
force placed directly on feet that are even slightly off-balance can result in pain or injury.
Other common causes of foot pain can include:
· Complications with the arch
· Achilles tendinitis
· Arthritic damage
· Not using the toes to help support pressure on the feet during activity
Ways to Alleviate Foot Pain

Our therapists will develop a treatment plan based on the symptoms presented with your foot pain. Physical therapy commonly focuses on improving muscle strength and flexibility of the feet to better support the body during movement. PT also focuses on improving the range of motion for feet, which may include changes to your walking method. Many patients are able to obtain relief for their feet and see a noticeable improvement in their physical ability that can provide lifelong relief.
Physical Therapy for Ankle Pain
Ankle Pain
Unfortunately, the ankle is one of the most commonly injured areas of the body. Because the ankles carry your entire weight during the majority of physical activity, it is very vulnerable to injury and thus pain. Even something as simple as stepping down with the ankle bent incorrectly can cause muscular damage and result in pain. 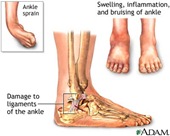
The ankle houses a large number of ligaments, tendons, and muscles all working together to move the joint during motion. Individually these pieces can be injured easily, leaving you with a constant source of pain and limited use of your ankle. Physical therapy (PT) seeks to provide pain relief for your ankle while working to return full functionality to have you back on your feet in no time.
Causes of Ankle Pain
One of the most general causes of ankle pain is a sprain in the ankle, which is one of the more common injuries suffered by those who lead active lives. Sprained ankles result from an overstretching of the ligament, creating either a complete or partial tear in the ligament. The severity of the sprain is directly linked to the size of this tear. Ankle sprains can cause a large amount of pain and will inhibit your ability to use your ankle. 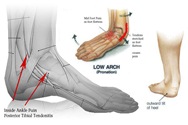
Other conditions that may cause you to feel pain in the ankle may include:
· Arthritic inflammation
· A stress related fracture
· Pain that results from a complication in the foot
Physical Therapy for Ankle Pain
Treating Ankle Pain
Our physical therapists are well versed in the treatment of ankle pain and will be able to provide you pain relief while helping restore functionality to your ankle. Treatments used will be based on the origin of your pain, and may include rehabilitation, medication, stretching exercises, and strength training to better prevent a future injury. One of the best things you can do for your ankle prior to our treatment is to keep weight off of it as much as possible in order to let the muscles rest.
Physical therapy for Achilles Pain
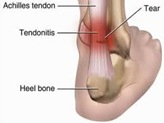 Injury to the Achilles tendon can produce pain located in the back of the leg near the heel. The Achilles tendon connects the heel bone to the calf muscles.
Injury to the Achilles tendon can produce pain located in the back of the leg near the heel. The Achilles tendon connects the heel bone to the calf muscles.
This tendon is the primary muscle used while walking, running, and jumping and is prone to inflammation due to degeneration and overuse. Inflammation in the Achilles tendon can lead to swelling, irritation of the area, and pain for the patient as it is the body’s largest tendon.
Physical Therapy For Achilles Tendon Pain
Types of Achilles Tendinitis
There are two types of Achilles inflammation, separated by the area of the tendon that becomes inflamed.
Noninsertional Achilles tendinitis (inflammation) occurs in the middle of the tendon where muscle fibers have begun to break down. This gradual degradation occurs primarily from the tendon’s overuse, making noninsertional Achilles tendinitis a commonly seen injury for active youth.
Insertional Achilles tendinitis occurs in the lower part of the heel, where the tendon meets and attaches (inserts) inside the bone of the heel.
In both insertional and noninsertional tendinitis, the damaged Achilles tendon fibers have the potential to calcify (harden) leading to further pain felt in the heel. Bone spurs, which are extra growth of bone that form into jutting pieces, may also form. Bone spurs are seen more commonly with insertional Achilles tendinitis, mainly due to inflammation occurring in the heel bone. Insertional Achilles tendinitis can occur in any patient regardless of their activity level.
PT For Achilles Tendinitis
Physician Evaluation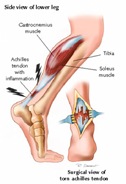
After examining what symptoms presented by the patient, the physician will physically examine the foot and ankle. During examination, the physician will check for swelling on the Achilles tendon and check for a thickening or enlargement of the tendon. Bone spurs will also be examined for. The physician will make note of where pain is indicated, checking primarily the middle of the tendon and the back of the heel. The current range of motion for the ankle will also be taken, with special attention paid to any reduction in the normal range of motion.
Best PT for Achilles Pain
Other symptoms of Achilles Pain may include:
• Pain and stiffness of the tendon
• Intense pain after exercise or exertion
• Swelling that increases throughout the say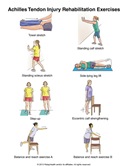
A “pop” in the heel or back of calf may indicate a rupture of the Achilles tendon and should be immediately be seen by a doctor.
Treatment for Achilles Pain
Although it seems more effective with noninsertational tendinitis, patients have found success in the elimination of Achilles pain symptoms with physical therapy. Innovative studies on new therapy techniques have been conducted by the Centre for Sports and Exercise Medicine, Queen Mary University of London, and show great promise in a full recovery of acute and chronic Achilles Tendinopathy (AT) and associated Achilles pain.
It is crucial to correctly attend to an injury with a proper treatment and physical therapy plan. Scientific evidence now supports the theory that what is many times considered an “Acute Tendinopathy” is actually an improperly healed chronic injury without histonic or biochemical inflammation that could have lifelong implications and increase in severity.
If you are experiencing Achilles pain, please contact ActveCare Physical Therapy.
Karena Wu on CBS Fit Minute November 19, 2013
Karena demonstrates the Plank with Leg Lifts. A great move for the core and hips as we start the winter season!
Direct link here
How Chefs Stay Fit and Sane
By Channaly Philipp, Epoch Times | November 2, 2013
How do chefs handle the pressures of the kitchen? We spoke with several chefs who shared how they handle the heat.

Flinty tempers, frayed nerves, fire, potential explosive situations. The restaurant kitchen is filled with dramatic stuff that reality TV producers dream of.
But from a chef’s perspective, there’s another reality: that of trying to find time to eat well while being around food all the time, working while hunched over all day, in sweltering kitchens, day after day, and not letting one’s body go to pot in an industry known for working long, hard, hot hours. And, also, in the middle of the hectic environment, how to keep one’s sanity.
How do chefs handle the pressures of the kitchen? We spoke with several chefs who shared how they handle the heat.
When chef Wylie Dufresne describes the injuries he has sustained over 30 years in food industry (he’s now 43 and started at 11), it sounds like a medical chart rundown: plantar fasciitis in the feet, knees slowly giving out; hip problems; tearing both hamstrings (due to an injury while playing softball but exacerbated by the tightness in his legs, he said); tightness in his lower back, from 20 years spent hunched over; a herniated disk in his back; shoulder surgery; neck problems; with the most chronic injuries in both his forearms, tennis elbow and golfer’s elbow.
He says he is at one end of the spectrum in terms of the number of injuries, but that sustaining chronic injuries is not unusual for any chef who’s been in the industry by the time they’ve spent 20 years working.
Finding the time to carve out for chefs is extremely hard, said Dufresne’s physical therapist Karena Wu, who has been treating him since 2004, once a week for maintenance, but more often as injuries call for it.
More often than not, the first thing she knows that chef clients do at the end of their shift, late a night, is to get a drink. “It’s like a snowball effect. You’ve worked 12 to 14 hours, which is a really long shift and you have a cocktail, which depresses your system.”
It doesn’t do anything positive for the body, she said, except to provide a brief break mentally. “It’s not going to help motivate you in the morning to go for a run and stretch or do some strength training before you start your shift again.”
For Dufresne, it’s only been recently, with marriage and parenthood of children ages 1 and 4, that he’s tried to find a balance, and he strives to stay fit so he can be as healthy as possible—working out and biking to work— when he does get to spend time with his family. “It’s when I’m running after a 4-year-old and I’m not winded that I see the value of [fitness].”
Before that, the usual routine of working all day and then going out eating and drinking and going to sleep worked well for him. “That’s all you do for many, many years and you do that very happily.”
When he does get some time off just to himself, he unwinds by going to the movies, which enables him to sit in the dark and not think of many things, he said.
“As you get older and you have a family it gets harder to find those moments. But is also gets more important. It’s about balance but for me, when I’m not working I want to spend as much time as I can with my family. That’s restorative as well.”
The Push-up Guy
Some chefs might look for an outlet that takes them far from the world of the kitchen, while for others, just the opposite is true.
Anthony Martin, 33, executive chef at Tru in Chicago, has followed a disciplined regimen for about seven years that he never fails to miss: he wakes up, checks email, and launches into an hour’s intense workout at home, to the tune of 25 push-ups a minute and 1,000 push-ups per session.
It’s not just a physical workout, though. It’s during this crucial hour that his creativity comes out, so he keeps a menu close by to make notes.
“The more I get into the workout, the more strenuous it is, the more active my thoughts get,” he said.
On some days, he ends up with about 30 new dishes sketched out.
“My whole day revolves around what I get done in that hour. The rest of the day revolves around making those ideas come to light,” he said.
The Boxer
For chef Chris Santos (Beauty & Essex, The Stanton Social), traditional gym workouts just don’t work for him. His passion is boxing, and he trains at Gleason’s Gym in Brooklyn, alongside boxing pros—the equivalent of training at basketball with the Knicks, if you could.
Santos grew up watching boxing at his grandfather’s knee and has been training seriously since 1993.
He harbors no thoughts of payroll when he’s boxing, he’s wholly focused. He gets “crazy strength from doing this. And there’s no way I’m eating garbage food and drinking a bunch of beer. It keeps me on point.”
The Meditator
Whereas some chefs seek relief in activities that are equally intense or adrenaline-driven as the kitchen, Zizhao Luo, the executive chef at Radiance Fine Asian Cuisine, takes another path: meditation. Luo, who is his mid-40s, values the tranquility that it gives him.
He believes being both healthy and calm is responsible not just to himself but to his customers too.
“When a chef is calm,” he said, “The calmer he is, the better the dish he’s able to make.”
Luo wakes up shortly before 5:00 every morning to practice the meditation and exercises of Falun Dafa, an ancient Chinese body-mind practice. He is one of only a couple of chefs whom I interviewed who felt no chronic pain or aches anywhere in their bodies.
He strives to keep a positive and uplifting spirit, and be understanding of others. With that mindset, “Stressful situations don’t become a burden.”
Luo was an accomplished and recognized chef long before he started meditating. He was somewhat of a young prodigy, taking up the position of executive chef of Kai Kong, one of Beijing’s most prestigious hotels, at the age of 21.
But, Luo said, after he started practicing Falun Dafa, the way he viewed and used his wok, his tools, the ingredients around him all became connected. “I feel everything is connected,” he said. Luo’s translator elaborated, saying that the meaning is that everything is connected as if it’s all one, single body.
The Surfer
With the beach a block away from his front door in Manhattan Beach, Calif., Keith Roberts, 58, chef at the Loews Hotel Santa Monica, doesn’t have to go far to hit the waves.
“Surfing is a very physically demanding sport. It’s the only sport you have to work for before you get to have fun,” he said.
Years ago he gave up smoking as a New Year’s resolution. But he then put on 40 pounds within a year and a half. He needed to work out and lose the weight but an obstacle stood in his way. “I needed to find a gym between the restaurant and the bar,” he said. It was all too easy to grab a couple of beers after work (“a couple of beers makes you hungrier so that means more weight, too.”)
For his following New Year’s resolution, he gave up drinking. These days, he’s not a teetotaler, but if he goes out and has a couple of drinks, he finds he’s too tired to go surfing in the morning. “The love of surfing drives a lot of it. The whole picture of staying in shape, it keeps me in better health, I’m a better husband, a better father. It all fits together.”
The Sharpener
When Chef Carmen Rodriguez (executive chef at Fuego! in Santa Fe), 45, recalls the days of cooking with an M-16 on his shoulder when deployed in the field—his last tour of duty was in the Air Force in Egypt right before Desert Storm, the pressures of the kitchen seem to recede. He was feeding the hundreds and thousands of troops in unfriendly places. Somehow, even his busiest nights at Fuego! just can’t compare.
“Most kitchens are hectic and utter chaos,” he said. “I don’t allow that craziness in my kitchen.” He makes a point of teaching all his staff how to handle themselves on the line.
He was diagnosed as a diabetic and said he ignored it for a long time, until he couldn’t anymore. “I wanted to be around to dance at my daughter’s wedding,” and he’s ever since cut back on processed foods and animal fats. He also works out six days a week.
Rodriguez also has an unusual practice that centers him.
“I do meditate. I don’t go home and watch television. I don’t go home and down a bottle of scotch. I sharpen my knives.” He pulls out his large collection, gives them a hot water bath and sharpens them. “It clears everything out of your head. That repetitive motion relaxes me.” He does this for two hours, whenever he needs to, often once a week.
The Ultra Marathoner and Yogi
Chef Gregory Gourdet (Departure) in Portland (by way of New York) remembers clearly the days of yore, when he’d order a bacon cheeseburger and mac ‘n’ cheese at 2 a.m. “I can’t even imagine doing that now.”
For Gourdet, it’s all about making conscious decisions. He’s been on the paleo diet for some time now, and as an inveterate runner, recently completed a 50-mile race. “It was supposed to be 100 miles.” Still, he knew if he set his goals high, he would make some progress on his goal.
He takes into account the seasons his restaurant goes through—taking advantage of less busy times to set fitness goals for himself.
Last year, during an insanely busy summer season, he found he had gained 20 pound in four months. “By the end of September, I was overweight, sluggish, tired, my back started hurting.”
It was so busy he’d stopped his yoga and strength training. He told himself he “should go on an exercise bender” and posted a challenge on Facebook to others in the industry in Portland: exercise for 30 days in a row, for 30 minutes a day, up until Thanksgiving. “It’s great community support,” he said, and makes fitness fun. This year’s challenge just started this past Tuesday.
He finds working out a great way to “let the night go and have some personal time.”
“Even at a busy gym, I can still find a place I know that’s better for me. I have a sense of stillness. I’m taking myself out of my work environment and challenging myself in a different way and achieving my goal there. It sets the tone for the rest of your day.”
Yoga is also important to him to help his back and opening up the front of the body. “When you’re on your feet all day, hunched over, also your wrists and your arms, it’s really kind of brings your body down.”
Cooking as Therapy
Chef Einat Admony (Babaloosta, Taim), 42, relishes the beauty of the outdoors and started running at her local park in Fort Greene this past summer.
But her favorite exercise is boxing. She once had a session with her trainer, but had just had a fight and was feeling upset. “My trainer said, ‘I think I have something for you.’ He brought out a pair of gloves. “I like that I can punch,” she said. It offers her relief and a good cardio workout, and it makes her refreshed when she gets into the kitchen.
As for what keeps her happy and balanced, she said, “Cooking is my therapy.” After a 12-hour day at the restaurant, she gets home and still wants to cook. When she is stressed, she cooks. Preparing Friday night Shabbat dinners for anywhere from 10 to 20 people is a tradition.
Having two children also encourages her to prepare healthier home meals that include a lot of vegetables. “My kids are carnivores,” she said.
Marathon Tips from Karena, Published in the Epoch Times Nov 2, 2013
For all of the marathon runners, congratulations on your accomplishment. Hope you were able to catch the last minute tips from Karena Wu. Her article below was published in the Epoch Times to help you out before the race. If you missed it, save it for your upcoming marathons and happy training!
_____________________________
10 Tips for Marathon Runners
The NYC marathon is rapidly approaching. For those running, this last week is essential. I am a physical therapist in Manhattan; I’ve treated world-class runners including Maurelhena Walles (one of the top ranked sprinters in the world), and as a runner myself, I have some advice for marathon runners:
Diet
Carbo-load, don’t fat load. During the last three days, make sure your calories emphasize carbs, which is what fuels you on race day.
Footwear
Select the shoes and socks you’ll wear in the marathon. Test them with at least one 10-mile run to make sure you don’t blister.
Distance
Two weeks prior to the race is when you should taper distance and intensity. Eliminate long and hard runs and in the last week, do 30-50 percent. No running daily! Two days right before, no running. Some people also prefer not to run the entire week prior.
The goal of the taper is to get your body rested to maximize it’s potential during the race!
Warm-up
Before long runs warm up by walking or doing a very light jog (slower than your pace) for no more than 10 minutes. Finish with stretching.
Stretching
Start Loose: 10-15 minutes before the start of the race, get your muscles warmed up with gentle stretches, especially as you are herded to the start. You can also include a light jog.
Start Slow
For the first 2-3 miles, it’s ok to start a little slower to conserve your glycogen. Then pick up the pace to what you trained for.
Race Drinks
Practice refueling with sports drinks and gels that you know will be on the race course. Find out the distance between stations and practice drinking at the rate in between stations.
Stay on Pace
Relax. With the energy of the start of the race and with thousands of people around you, you might go too hard too fast so it’s better to stick to your game plan to know what works best for you. Stay on pace.
Mind Games
Sing a song to yourself as you run, it helps cover distance and time.
Motivate Yourself
Around mile 23, tell yourself what you’ve accomplished and that you will finish. It helps you mentally to know that you can finish and that the pain is temporary. You’ve put the work in and now you just have to finish that finish line!
NYC Physical Therapist Karena Wu is a graduate from the Program in Physical Therapy at Columbia University and owner of ActiveCare Physical Therapy. She takes a holistic approach and utilizes advanced manual therapies, Kinesiology Tape, and Pilates for rehabilitation www.bestptnyc.com.
Best PT NYC 2013 welcomes Joe Castelli
 Joseph J. Castelli Jr, is a native of Brooklyn, New York. He received a Bachelor of Science in Finance from St. John’s University in New York. He then went on to receive a Bachelor of Science in Physical Therapy from SUNY at Stony Brook in New York. In December 2011, received his Transitional Doctorate of Physical Therapy from the University of Colorado’s School of Medicine in Denver, Colorado. Joe has over 14 years of experience as a Physical Therapist. He works as a consultant and independent contractor. He has taken advanced manual therapy courses following Stanley Paris at the University of St. Augustine and Myofascial manual therapy from Hands On Seminars in New York. Joe is Certified as an Ergonomic Assessment Specialist as well as a Credentialed Clinical Instructor with the American Physical Therapy Association.
Joseph J. Castelli Jr, is a native of Brooklyn, New York. He received a Bachelor of Science in Finance from St. John’s University in New York. He then went on to receive a Bachelor of Science in Physical Therapy from SUNY at Stony Brook in New York. In December 2011, received his Transitional Doctorate of Physical Therapy from the University of Colorado’s School of Medicine in Denver, Colorado. Joe has over 14 years of experience as a Physical Therapist. He works as a consultant and independent contractor. He has taken advanced manual therapy courses following Stanley Paris at the University of St. Augustine and Myofascial manual therapy from Hands On Seminars in New York. Joe is Certified as an Ergonomic Assessment Specialist as well as a Credentialed Clinical Instructor with the American Physical Therapy Association.
Best PT NYC 2013 welcomes Mila Grinberg
 Mila Grinberg earned her Doctorate of Physical Therapy from Hunter College, CUNY. As a practitioner, she is committed to providing quality patient care, with an emphasis on manual and functional therapy. Mila believes in personal growth and pursues ongoing professional development.
Mila Grinberg earned her Doctorate of Physical Therapy from Hunter College, CUNY. As a practitioner, she is committed to providing quality patient care, with an emphasis on manual and functional therapy. Mila believes in personal growth and pursues ongoing professional development.Mila has a background in dance performance and instruction, which gives her first-hand experience with injuries and injury prevention and an appreciation of movement quality. She is excited to be a part of the ActiveCare Physical Therapy team!
 ActiveCare Physical Therapy, PC
ActiveCare Physical Therapy, PC
12 W 37th St. Ste. 1202
New York, NY 10018



 Click to watch video
Click to watch video
