About ActiveCare Physical Therapy®
The Best Physical Therapists in NYC
-
Our therapists are licensed in New York State and active members in the American Physical Therapy Association. We have advanced training in joint mobilization and myofascial release techniques.
-
We are dedicated practitioners with a passion for the profession and a comprehensive, holistic approach to treatment and healing. We treat each patient as an individual and treat the whole person, with a plan of care designed to meet the patient’s set goals for health, functionality and a return to work, tasks and activities. We network with a team of physicians, chiropractors, acupuncturists and massage therapists in order to provide guidance to other modalities that may be effective in the patients’ care. We also offer superior Telehealth services for physical therapy.
-
Physical Therapist and owner Dr. Karena Wu PT, DPT, OCS is a graduate of the Program in Physical Therapy at Columbia University and is affiliated with several healthcare organizations in New York City. She is certified as a Strength and Conditioning Specialist, Kinesio Taping Practitioner and Pilates Instructor, and uses SpiderTech Taping. She is also a Certified Orthopedic Manual Therapist, Strength and Conditioning Specialist, Graston Technique® Specialist and Pilates Instructor. She holds LSVT BIG, FMS and SFMA Level 1 certifications as well. Dr. Wu also specializes in vertigo and temporomandibular joint disorders.
-
ActiveCare is primarily an out-of-network facility. We accept all insurance with out-of-network benefits and file for most major insurance plans. We work with all prospective patients to create workable payment plans regardless of insurance coverage.
-
ActiveCare accepts Medicare, No-Fault and Workers Compensation patients depending on schedule availability.
-
ActiveCare’s administrators provide seamless and efficient concierge-style client service to all of our patients. And the whole ActiveCare team makes sure your time with us is a beneficial, productive and enjoyable experience.
Quick Links
Manual Therapy Bursitis Plantar Fascitis Meniscus Tears Labral Tears Kinesiology Taping Pilates Rehab
Visit Our Main Website:
www.ActiveCarePhysicalTherapy.com
Blog Posts Are Below:
* We Accept Medicare | No Fault | Workers Comp *
ActiveCare Welcomes New Physical Therapist Dr. Nikita Sak, DPT
 Dr. Nikita Sak is a dedicated physical therapist who is committed to helping patients restore function, improve mobility, and achieve their personal health goals. Born and raised in St. Petersburg, Florida, Nikita is the son of Ukrainian immigrants whose hard work and perseverance helped shape his strong work ethic and compassionate approach to patient care.
Dr. Nikita Sak is a dedicated physical therapist who is committed to helping patients restore function, improve mobility, and achieve their personal health goals. Born and raised in St. Petersburg, Florida, Nikita is the son of Ukrainian immigrants whose hard work and perseverance helped shape his strong work ethic and compassionate approach to patient care.
Nikita earned his Doctor of Physical Therapy degree from Florida Gulf Coast University, where he developed a deep appreciation for evidence-based practice and lifelong learning. His clinical education reinforced his passion for delivering individualized treatment plans that address each patient’s unique needs, challenges, and goals.
Throughout his career, Nikita has gained experience treating a wide range of orthopedic conditions, including post-operative rehabilitation following total joint replacements, rotator cuff injuries, sports-related injuries, and chronic musculoskeletal disorders. He has also worked with patients recovering from neurological conditions such as stroke, vestibular dysfunction, and spinal cord injuries, helping them regain confidence and independence in their daily lives.
Nikita believes that successful rehabilitation extends beyond physical recovery. He places a strong emphasis on empathy, patient education, and understanding the emotional and mental aspects of healing. His commitment to serving the community has included participation in fall-risk assessment programs for underserved populations in Southwest Florida. By building meaningful relationships with his patients, Nikita strives to create a supportive environment that empowers individuals throughout their recovery journey.
To schedule an appointment with Dr. Sak, call or email us today!
ActiveCare Physical Therapy™
29 West 38th Street, Suite 601
New York, NY 10018
Phone: (212) 777-4374
Email: staff@bestptnyc.com
Sciatica and Back Pain Relief Starts Here
Lower back pain and sciatica can affect people of all ages, from students and busy professionals to athletes and older adults. Physical therapy can help relieve pain and improve mobility without medications or surgery.
Sciatica happens when the sciatic nerve becomes irritated, causing pain, tingling, or numbness that travels from the lower back down the leg. Physical therapy helps reduce irritation, restore movement, and strengthen the muscles that support the spine and improve posture.
“At ActiveCare Physical Therapy, we treat the root cause of pain, not just the symptoms,” says Dr. Karena Wu, Clinical Director and Owner of ActiveCare PT. “Our goal is to help patients of all ages move with confidence and return to the activities they enjoy.”
Ready to Feel Better?
ActiveCare Physical Therapy creates personalized treatment plans to help patients move better, feel stronger, and get back to daily life with less pain and discomfort.
Book your evaluation today and start your recovery journey!
ActiveCare Physical Therapy™
29 West 38th Street, Suite 601
New York, NY 10018
Phone: (212) 777-4374
Email: staff@bestptnyc.com
How Manual Therapy and Cold Laser Therapy Work Together to Support Recovery
At ActiveCare Physical Therapy, combining manual therapy with low-level cold laser therapy can help support recovery by reducing pain, improving mobility, and promoting tissue healing. Hands-on treatment helps restore joint and soft tissue mobility, decrease muscle tension, and improve movement patterns, while cold laser therapy may help calm inflammation and support the body’s natural healing response. Together, these therapies can help patients feel more comfortable during exercise and daily activities.
“Combining skilled manual therapy with evidence-based technology allows us to help patients move more comfortably and recover more efficiently,” says Dr. Karena Wu, Owner and Clinical Director of ActiveCare Physical Therapy.
To learn whether manual therapy and laser therapy may be right for you, contact ActiveCare Physical Therapy at 212-777-4374 to schedule an evaluation.
ActiveCare Physical Therapy™
29 West 38th Street, Suite 601
New York, NY 10018
Phone: (212) 777-4374
Email: staff@bestptnyc.com
Core strengthening and why it’s important
Core strengthening is important because the core muscles provide stability, support posture, protect the spine, and help the body move efficiently during both daily activities and athletic performance. While many people associate the core only with abdominal muscles or achieving a toned midsection, the core is actually a complex group of muscles that work together to stabilize the entire body.
Weak core muscles can contribute to back pain, poor posture, balance problems, and increased injury risk. Physical therapy often includes core strengthening exercises because a strong and stable core is essential for long-term musculoskeletal health and functional movement.

What Is the Core?
The core includes far more than just the “six-pack” abdominal muscles. It consists of several muscle groups that stabilize the spine, pelvis, and trunk.
- Deep abdominal muscles (transverse abdominis)
- Obliques
- Rectus abdominis
- Lower back muscles
- Pelvic floor muscles
- Diaphragm
- Hip stabilizers and gluteal muscles
These muscles work together to support posture, control movement, and transfer force throughout the body.
Why Core Strength Matters
A strong core serves as the foundation for nearly every movement the body performs. Whether sitting, standing, walking, lifting, or exercising, the core helps stabilize the spine and maintain proper alignment.
Spinal Support and Back Pain Prevention
Weak core muscles can place excessive stress on the spine and surrounding joints. This often contributes to lower back pain and muscle fatigue. Strengthening the core helps distribute forces more evenly and improves spinal stability.
Improved Posture
Strong postural muscles help keep the body properly aligned. Core weakness often leads to slouching, forward head posture, and excessive strain on the neck and shoulders.
Better Balance and Stability
The core plays a major role in maintaining balance and controlling movement. Improved core stability can reduce fall risk and improve coordination during daily activities and sports.
Enhanced Athletic Performance
Athletes rely heavily on core strength for power generation, agility, and movement efficiency. A stable core improves running mechanics, lifting performance, and rotational control.
Common Signs of a Weak Core
Many people do not realize they have poor core stability until symptoms develop.
- Frequent lower back pain
- Poor posture or slouching
- Difficulty balancing
- Hip or pelvic instability
- Neck and shoulder tension
- Fatigue during prolonged standing or activity
Physical therapists often identify weak core activation patterns during movement assessments and posture evaluations.
How Physical Therapy Helps Improve Core Strength
Physical therapy focuses on retraining the core muscles to activate properly and work together efficiently. Rather than simply performing high-repetition abdominal exercises, therapists emphasize controlled movement and proper muscle engagement.
Deep Core Activation
Therapists often begin by teaching patients how to activate the deep stabilizing muscles of the abdomen and pelvis. Proper breathing patterns and alignment are important components of this process.
Progressive Strengthening Exercises
As stability improves, exercises become more challenging and functional. These may include planks, bridges, dead bugs, bird-dogs, and Pilates-based movements.
Movement Re-Education
Core strengthening is integrated into real-life movement patterns such as squatting, lifting, walking, and reaching. This helps patients use their core effectively during everyday activities.
Core Strengthening Beyond Exercise
Improving core strength is not limited to workouts. Daily habits also affect core stability and posture.
- Maintaining proper sitting posture
- Avoiding prolonged slouching
- Using ergonomic workstations
- Practicing good lifting mechanics
- Staying physically active throughout the day
Consistent movement and postural awareness help reinforce the benefits of strengthening exercises.
Who Benefits from Core Strengthening?
Nearly everyone can benefit from improving core stability, including:
- Individuals with chronic back pain
- Office workers with poor posture
- Athletes seeking performance enhancement
- Older adults improving balance and fall prevention
- Post-surgical patients rebuilding stability
- Pregnant and postpartum individuals
Core training is highly adaptable and can be modified for different ages, fitness levels, and medical conditions.
Conclusion
Core strengthening is important because the core muscles support posture, stabilize the spine, improve balance, and protect the body during movement. Weak core muscles can contribute to pain, poor movement mechanics, and increased injury risk. Physical therapy provides a structured and personalized approach to improving core stability through targeted exercises, movement training, and postural correction.
Building a stronger core not only improves physical performance but also supports long-term musculoskeletal health and everyday function.
Contact Information
ActiveCare Physical Therapy™
29 West 38th Street, Suite 601
New York, NY 10018
Phone: (212) 777-4374
Email: staff@bestptnyc.com
What to expect at your first PT visit
 What to expect at your first PT visit is a common question for patients starting physical therapy for the first time. Whether you are recovering from surgery, managing chronic pain, or treating a sports injury, your first physical therapy appointment is designed to evaluate your condition, identify movement limitations, and create a personalized treatment plan to help you recover safely and effectively.
What to expect at your first PT visit is a common question for patients starting physical therapy for the first time. Whether you are recovering from surgery, managing chronic pain, or treating a sports injury, your first physical therapy appointment is designed to evaluate your condition, identify movement limitations, and create a personalized treatment plan to help you recover safely and effectively.
At ActiveCare Physical Therapy™ in New York City, the first visit is focused on understanding the whole patient—not just the injury. This comprehensive approach helps physical therapists identify the root causes of pain and develop a strategy for long-term improvement.
Why the First Physical Therapy Visit Is Important
The first session establishes the foundation for your entire rehabilitation program. During this appointment, the physical therapist gathers detailed information about your symptoms, movement patterns, posture, strength, and mobility.
This evaluation helps determine:
- The likely cause of your pain or dysfunction
- What activities or movements are contributing to symptoms
- Which muscles or joints need attention
- What treatment approach will be most effective
A thorough assessment also allows therapists to track your progress over time and adjust treatment as you improve.
Medical History and Discussion
Your appointment will usually begin with a conversation about your medical history and current condition.
Questions Your Therapist May Ask
The therapist may ask about:
- When your symptoms started
- Activities that worsen or improve your pain
- Previous injuries or surgeries
- Your work environment and daily activities
- Your exercise habits and lifestyle
These questions help the therapist understand how your symptoms affect your daily life and identify patterns that may contribute to the problem.
Physical Evaluation and Movement Assessment
After discussing your history, the therapist performs a detailed physical examination. This portion of the visit helps identify movement dysfunctions, muscle imbalances, and mobility restrictions.
Posture Assessment
Your therapist may evaluate how you sit, stand, and move to identify postural issues contributing to pain or tension.
Range of Motion Testing
Joint mobility and flexibility are measured to determine whether movement restrictions are present.
Strength Testing
Specific muscles may be tested to identify weakness or compensation patterns.
Functional Movement Analysis
You may be asked to perform movements such as squatting, walking, bending, or reaching so the therapist can observe how your body moves during real-life activities.
Your First Treatment Session
In many cases, treatment begins during the first visit. Depending on your condition, the therapist may use a combination of techniques to start reducing pain and improving mobility.
- Manual therapy to reduce muscle tension and improve joint mobility
- Gentle stretching or mobility exercises
- Postural correction strategies
- Education about movement habits and activity modifications
- Home exercises to begin improving strength and flexibility
The initial treatment is usually designed to introduce the body to therapy gradually without overloading irritated tissues.
What to Wear to Your Appointment
Comfortable clothing is recommended for physical therapy sessions. Since movement assessments are often part of the evaluation, it’s best to wear clothes that allow easy movement and access to the area being treated.
For example:
- Shorts for knee or hip injuries
- Tank tops or loose shirts for shoulder or neck issues
- Athletic shoes for gait and balance assessments
Questions You Should Ask Your Physical Therapist
Your first visit is also an opportunity to better understand your condition and recovery process. Helpful questions may include:
- What is likely causing my symptoms?
- How long will recovery take?
- What activities should I avoid?
- What can I do at home to improve my condition?
Open communication helps build a strong therapist-patient relationship and ensures you understand your treatment goals.
What Happens After the First Visit?
At the end of your appointment, your therapist will usually outline a treatment schedule based on your condition and goals. Many patients attend physical therapy one to three times per week depending on the severity of the issue.
Consistency with both in-clinic sessions and home exercises is one of the most important factors in achieving successful outcomes.
Conclusion
Understanding what to expect at your first PT visit can help reduce anxiety and prepare you for a successful rehabilitation experience. The first session focuses on evaluation, education, and beginning a personalized treatment plan designed to restore movement and reduce pain.
Physical therapy is a collaborative process, and starting with a thorough assessment allows therapists to create targeted strategies that support long-term recovery and improved function.
Contact Information
ActiveCare Physical Therapy™
29 West 38th Street, Suite 601
New York, NY 10018
Phone: (212) 777-4374
Email: staff@bestptnyc.com
ActiveCare Physical Therapy Participates in the Arthritis Foundation 2026 “Let’s Make Moves” Walk
Dear Friends,
ActiveCare Physical Therapy is proud to participate in this year’s Arthritis Foundation “Let’s Make Moves” Walk on Saturday, May 16th at 9:00 AM at Foley Square (60 Centre Street, NYC).

We would love for you to join the ActiveCare PT team for the walk, or support this important cause with a donation of any amount. Arthritis is the #1 cause of disability in America, and your support helps fund research, advocacy, and resources for millions living with this disease.
Join our team or donate here:
https://events.arthritis.org/teams/41602
Every contribution makes a difference. Here’s what your support can do:
- $500 helps address the shortage of rheumatologists by funding new fellowships
- $200 helps advocate to remove barriers to care such as high treatment costs and medication access
- $100 helps advance research for better treatments to reduce arthritis pain and improve mobility
- $50 helps provide education, camps, and resources for the 300,000 children living with arthritis
- $30 helps provide educational tools and resources for the 1 in 4 Americans affected by arthritis
No matter the amount, your support matters and moves the mission forward.

Thank you for joining us in this fight against arthritis!
Warm regards,
ActiveCare Physical Therapy
29 West 38th Street
Suite 601
New York, NY 10018
(212) 777-4374
Do Not Ignore Knee Pain
Knee pain can affect anyone, from runners and marathoners to active adults and older individuals. It can develop from overuse, muscle weakness, joint wear, or poor movement patterns. Taking care of your knees through proper strength, mobility, and early attention to discomfort can help you stay active and avoid long term problems.

“Many people wait until knee pain becomes severe before seeking help, but early attention to strength, flexibility, and movement mechanics can prevent much bigger issues later,” says Dr. Karena Wu, Owner and Clinical Director of ActiveCare Physical Therapy.
Do not ignore knee pain. Reach out to ActiveCare PT and take the first step toward stronger, healthier knees.
ActiveCare Physical Therapy™
29 West 38th Street, Suite 601
New York, NY 10018
Phone: (212) 777-4374
Email: staff@bestptnyc.com
https://activecarephysicaltherapy.com
Balance and fall prevention
 Balance and fall prevention are critical components of maintaining mobility, independence, and long-term health, especially as people age or recover from injury. Falls are one of the leading causes of injury among older adults, but balance problems can affect people of all ages due to neurological conditions, muscle weakness, injuries, or vestibular disorders. Physical therapy plays a major role in improving balance, reducing fall risk, and helping individuals move with greater confidence and stability.
Balance and fall prevention are critical components of maintaining mobility, independence, and long-term health, especially as people age or recover from injury. Falls are one of the leading causes of injury among older adults, but balance problems can affect people of all ages due to neurological conditions, muscle weakness, injuries, or vestibular disorders. Physical therapy plays a major role in improving balance, reducing fall risk, and helping individuals move with greater confidence and stability.
At ActiveCare Physical Therapy™, balance training programs are designed to address the underlying causes of instability while improving strength, coordination, and body awareness.
Why Balance Is Important
Balance is the body’s ability to maintain stability while standing, walking, or performing movement. It relies on communication between several systems in the body, including:
- The vestibular system in the inner ear
- Vision and visual processing
- Muscles and joints providing proprioceptive feedback
- The nervous system coordinating movement responses
When one or more of these systems becomes impaired, balance problems can occur. This may lead to unsteadiness, dizziness, slower reaction times, and an increased risk of falling.
Common Causes of Balance Problems
Balance impairments can develop from a wide range of conditions and physical limitations.
Muscle Weakness
Weakness in the legs, hips, and core muscles can reduce stability and make it harder to recover from sudden movements or uneven surfaces.
Vestibular Disorders
Conditions affecting the inner ear, such as BPPV or vestibular neuritis, can cause dizziness and impaired balance.
Neurological Conditions
Stroke, Parkinson’s disease, neuropathy, and multiple sclerosis can interfere with coordination and movement control.
Joint Pain and Arthritis
Painful joints may alter walking patterns and reduce confidence during movement.
Poor Vision
Visual impairments make it more difficult for the body to orient itself in space and respond to obstacles.
Why Fall Prevention Matters
Falls can lead to serious injuries such as fractures, head injuries, and reduced mobility. Even when a fall does not cause major injury, it can lead to fear of movement and reduced physical activity, which often worsens balance over time.
Preventing falls is about more than avoiding accidents—it is about preserving independence, confidence, and overall quality of life.
How Physical Therapy Improves Balance
Physical therapists evaluate the specific factors contributing to instability and create personalized programs to improve balance and mobility safely.
Balance Retraining Exercises
Therapists use exercises that challenge the body’s balance systems in a controlled environment. These exercises help improve coordination, reaction time, and postural control.
Strengthening Programs
Improving lower body and core strength helps stabilize the body during walking and daily activities.
Gait Training
Walking mechanics are assessed to identify abnormalities that may increase fall risk. Therapists work on improving stride length, foot placement, and walking confidence.
Vestibular Rehabilitation
For patients experiencing dizziness or vertigo, vestibular physical therapy can help retrain the inner ear and nervous system to improve stability.
Simple Fall Prevention Strategies at Home
Small environmental changes can significantly reduce fall risk inside the home.
- Remove loose rugs and clutter from walking paths
- Ensure rooms and hallways are well lit
- Install grab bars in bathrooms if needed
- Wear supportive footwear with good traction
- Avoid rushing when changing positions or walking
Combining these safety measures with physical therapy can greatly improve overall stability and confidence.
Who Benefits from Balance Training?
Balance therapy is beneficial for many different individuals, including:
- Older adults concerned about fall risk
- Patients recovering from surgery or injury
- Individuals with vestibular disorders or vertigo
- People with neurological conditions affecting coordination
- Athletes recovering from lower extremity injuries
Even younger individuals can benefit from balance training to improve athletic performance and reduce injury risk.
Conclusion
Balance and fall prevention are essential for maintaining mobility, independence, and confidence throughout life. Whether balance problems are caused by weakness, injury, neurological conditions, or vestibular dysfunction, physical therapy provides effective solutions for improving stability and reducing fall risk.
Through personalized training programs, strengthening exercises, and movement retraining, patients can safely regain confidence in their ability to move and function independently.
Contact Information
ActiveCare Physical Therapy™
29 West 38th Street, Suite 601
New York, NY 10018
Phone: (212) 777-4374
Email: staff@bestptnyc.com
Website: https://activecarephysicaltherapy.com
Injury Prevention for Runners
 Injury prevention for runners is essential for maintaining consistent training, improving performance, and avoiding setbacks that can interrupt progress. Running is one of the most accessible and beneficial forms of exercise, but the repetitive nature of the sport places significant stress on muscles, joints, and connective tissues. Without proper preparation and recovery strategies, runners may develop overuse injuries that affect their ability to continue training.
Injury prevention for runners is essential for maintaining consistent training, improving performance, and avoiding setbacks that can interrupt progress. Running is one of the most accessible and beneficial forms of exercise, but the repetitive nature of the sport places significant stress on muscles, joints, and connective tissues. Without proper preparation and recovery strategies, runners may develop overuse injuries that affect their ability to continue training.
Physical therapy plays a major role in helping runners stay healthy by identifying movement imbalances, improving strength and mobility, and guiding runners toward safer training habits.
Why Running Injuries Are So Common
Running injuries often develop gradually rather than from a single traumatic event. The repetitive impact forces experienced with every stride can lead to cumulative stress on the body. When muscles become fatigued or movement patterns are inefficient, the risk of injury increases.
Many injuries occur when training intensity increases too quickly, when footwear is inappropriate, or when underlying muscle weaknesses go unaddressed. Physical therapists frequently see runners who unknowingly compensate for these issues until pain appears.
Common Running Injuries
Runners may experience a variety of musculoskeletal conditions, many of which are preventable with proper training and conditioning.
- Runner’s knee (patellofemoral pain syndrome)
- Shin splints (medial tibial stress syndrome)
- Achilles tendonitis
- Plantar fasciitis
- Iliotibial band syndrome (IT band syndrome)
- Stress fractures
These injuries typically arise from repetitive loading, muscle imbalances, and biomechanical inefficiencies.
How Physical Therapy Supports Injury Prevention
Physical therapists evaluate the way a runner moves to identify patterns that may contribute to injury risk. By analyzing posture, stride mechanics, flexibility, and muscle activation, therapists can develop targeted strategies to improve running efficiency.
Movement and Gait Analysis
A detailed gait assessment allows therapists to observe how the body absorbs impact with each step. Issues such as excessive pronation, hip drop, or poor knee alignment can often be identified and corrected through training and strengthening exercises.
Strength Training for Runners
Strong supporting muscles help absorb the forces generated during running. Weakness in the hips, glutes, and core can lead to excessive strain on the knees and lower legs.
Strengthening these areas helps stabilize the pelvis and improve stride mechanics, reducing injury risk.
Mobility and Flexibility Work
Tight muscles can limit range of motion and force the body to compensate during running. Improving flexibility in the hips, calves, hamstrings, and ankles helps maintain efficient movement patterns.
Training Load Management
One of the most common causes of injury is increasing mileage or intensity too quickly. Physical therapists help runners structure training plans that allow gradual progression while giving tissues time to adapt.
Key Strategies for Injury Prevention
Successful injury prevention requires a combination of smart training habits and body awareness.
- Gradually increase mileage and intensity
- Incorporate strength training into your weekly routine
- Prioritize proper warm-ups and cool-downs
- Wear appropriate running shoes and replace them regularly
- Listen to early warning signs such as persistent soreness or joint pain
Paying attention to these strategies can significantly reduce the likelihood of developing overuse injuries.
The Role of Recovery in Preventing Injuries
Recovery is just as important as training when it comes to injury prevention for runners. Adequate rest allows muscles and connective tissues to repair and adapt to training demands.
Active recovery activities such as mobility exercises, foam rolling, and low-impact cross-training can help reduce stiffness and maintain overall fitness while allowing the body to recover.
When Runners Should Seek Professional Help
If pain persists during or after running, it is important not to ignore the symptoms. Continuing to run through pain can worsen underlying issues and prolong recovery.
A physical therapist can evaluate the source of the discomfort and provide corrective strategies before the problem develops into a more serious injury.
Conclusion
Injury prevention for runners involves more than simply logging miles. Proper strength training, mobility work, running mechanics, and recovery strategies all play a role in keeping runners healthy.
Physical therapy provides valuable insight into movement patterns and helps address the underlying causes of injury risk. With the right guidance and training approach, runners can continue pursuing their goals while protecting their long-term musculoskeletal health.
Contact Information
ActiveCare Physical Therapy™
29 West 38th Street, Suite 601
New York, NY 10018
Phone: (212) 777-4374
Email: staff@bestptnyc.com
Website: https://activecarephysicaltherapy.com
2026 NYC Blizzard: Feeling It After the Snow?
After yesterday’s blizzard, many New Yorkers are shoveling snow, cleaning off cars, and walking carefully on icy sidewalks. These winter activities can strain not just your back, but also your shoulders, knees, and hips, especially in cold weather when muscles are tighter.

As Dr. Karena Wu, Clinical Director and Owner of ActiveCare PT, shares, “Cold weather and sudden physical demands can lead to soreness or injury if the body is not prepared.”
If you are feeling pain, stiffness, or discomfort after the storm, physical therapy can help you recover safely and prevent lingering issues.
Reach out to ActiveCare PT today to get back to moving comfortably and confidently this winter!
To schedule a physical therapy appointment, call or email ActiveCare Physical Therapy today.
ActiveCare Physical Therapy™
29 West 38th Street, Suite 601
New York, NY 10018
Phone: (212) 777-4374
Email: staff@bestptnyc.com
Website: https://activecarephysicaltherapy.com
Happy New Year from ActiveCare Physical Therapy!
Dear ActiveCare PT Family,
Happy New Year! We hope you had a wonderful holiday season and are feeling refreshed and ready for a fresh start.
As we head into the new year, we want to sincerely thank you for choosing ActiveCare PT and trusting us with your care. It truly means so much to our entire team.

The beginning of the year is a great time to check in with your body and your movement. Staying consistent with your exercises, keeping your body moving throughout the day, and paying attention to the small things can make a big difference over time. As owner and Clinical Director, Dr. Karena Wu, often reminds patients, “Meaningful progress comes from consistent, high quality movement and individualized care.”
As we move through January, you may hear from our front desk team about updating some routine paperwork, including insurance information and patient care contracts, as many plans renew at the start of the year. If you have any questions, Kanal, our Director of Business Development, is always happy to help.
Wishing you a healthy, happy, and active New Year! We look forward to continuing to work with you and supporting you in the months ahead.
Warmly,
The ActiveCare Physical Therapy Team
Back and Neck Pain From Desk Work
 Back and neck pain from desk work is one of the most common musculoskeletal complaints among office workers and professionals in New York City. Long hours spent sitting at a computer, poor workstation ergonomics, and prolonged forward head posture can place significant strain on the spine, leading to muscle tension, stiffness, and chronic discomfort. Fortunately, physical therapy can help address the underlying causes of desk-related pain and provide long-term relief.
Back and neck pain from desk work is one of the most common musculoskeletal complaints among office workers and professionals in New York City. Long hours spent sitting at a computer, poor workstation ergonomics, and prolonged forward head posture can place significant strain on the spine, leading to muscle tension, stiffness, and chronic discomfort. Fortunately, physical therapy can help address the underlying causes of desk-related pain and provide long-term relief.
Why Desk Work Causes Back and Neck Pain
Many people assume that sitting is a restful position, but sitting for long periods—especially with poor posture—can place continuous stress on the spine and surrounding muscles. Over time, this repetitive strain can lead to muscle imbalances, joint irritation, and reduced mobility.
Desk work commonly encourages a forward head position, rounded shoulders, and a slouched back. These positions increase the load on the cervical and thoracic spine and can lead to muscle fatigue and tension throughout the upper body.
Common Symptoms Associated with Desk-Related Pain
People who spend long hours at a desk often develop a predictable pattern of symptoms. These symptoms can appear gradually and worsen over time if not addressed.
- Persistent neck stiffness or soreness
- Aching between the shoulder blades
- Tension headaches
- Lower back pain after prolonged sitting
- Shoulder tightness or reduced mobility
- Numbness or tingling in the arms or hands
In many cases, these symptoms are not caused by a single injury but rather by repetitive postural stress that accumulates throughout the workday.
How Poor Ergonomics Contribute to Pain
Workstation setup plays a major role in whether desk work becomes harmful to the spine. When a desk, chair, keyboard, or monitor is positioned incorrectly, the body must compensate with awkward postures.
Monitor Position
If a computer monitor is too low, people tend to tilt their heads downward, increasing strain on the neck muscles.
Keyboard and Mouse Placement
When the keyboard or mouse is positioned too high or too far away, the shoulders elevate and the arms overreach, creating tension in the upper back and neck.
Chair Support
A chair without proper lumbar support can encourage slouching, which places excessive pressure on the lower back and spinal discs.
How Physical Therapy Helps Relieve Desk-Related Pain
Physical therapy focuses on addressing the root causes of back and neck pain from desk work rather than simply masking symptoms. A physical therapist evaluates posture, muscle imbalances, joint mobility, and daily movement habits to develop a personalized treatment plan.
Postural Correction
Therapists help patients understand proper sitting alignment and how to maintain it throughout the day. Small adjustments in posture can dramatically reduce stress on the spine.
Manual Therapy
Hands-on techniques can help release tight muscles in the neck, shoulders, and upper back. Manual therapy can also restore mobility in stiff joints that contribute to discomfort.
Strengthening Exercises
Weak postural muscles often contribute to desk-related pain. Strengthening the deep neck flexors, upper back muscles, and core stabilizers helps support better spinal alignment.
Mobility and Stretching Programs
Specific stretches and mobility exercises help counteract the stiffness that develops from prolonged sitting. These exercises are often designed to be performed during short breaks throughout the workday.
Simple Strategies to Reduce Desk Work Pain
While physical therapy is highly effective, daily habits also play an important role in preventing back and neck pain.
- Take movement breaks every 30–60 minutes
- Adjust your monitor so the top of the screen is at eye level
- Keep your feet flat on the floor while sitting
- Use a chair with proper lumbar support
- Perform gentle neck and shoulder stretches during the day
Even small ergonomic adjustments can significantly reduce the strain placed on your spine during long work hours.
When to Seek Physical Therapy
If back or neck pain from desk work persists despite improving your workstation setup, physical therapy may be necessary. Persistent stiffness, headaches, radiating pain, or reduced mobility are signs that deeper musculoskeletal issues may be developing.
Early treatment can prevent these issues from becoming chronic and help restore comfortable movement.
Conclusion
Back and neck pain from desk work is increasingly common as more people spend long hours working at computers. Poor posture, muscle imbalances, and improper workstation setup all contribute to spinal strain.
Physical therapy offers effective solutions by correcting posture, restoring mobility, strengthening supporting muscles, and teaching strategies to prevent recurring pain. With the right treatment approach, desk workers can remain productive while protecting their long-term spinal health.
Contact Information
ActiveCare Physical Therapy™
29 West 38th Street, Suite 601
New York, NY 10018
Phone: (212) 777-4374
Email: staff@bestptnyc.com
Website: https://activecarephysicaltherapy.com
Merry Christmas & Happy Holidays from ActiveCare Physical Therapy
As the year ends, the ActiveCare Physical Therapy team celebrates in front of a holiday tree decorated with ornaments signed by our patients. Each name represents trust, healing, and community.
Dr. Karena Wu, Owner and Clinical Director, says, “Seeing our patients’ names on the tree reminds us that true healing happens through connection and compassionate care.”

This season, keep moving with light activity and mindful posture. Physical therapy is not just for injuries, it is a proactive way to maintain strength and mobility. Schedule an evaluation to start the new year feeling your best.
Thank you for being part of the ActiveCare Physical Therapy community.
Merry Christmas & Happy Holidays from ActiveCare Physical Therapy!
__________________
ActiveCare Physical Therapy, PC
www.bestptnyc.com
29 West 38th Street, #601
New York, NY 10018
212-777-4374 office
212-901-6992 fax
917-916-0136 mobile
ActiveCare Physical Therapy, Pvt Ltd
Prabhadevi Industrial Estate
Unit No. 9, Ground Floor
Veer Savarkar Marg, Prabhadevi
Mumbai 4000215 India
+91-022-24220122 office
Meet Dr. Kiernan Monaco, PT, DPT
 Dr. Kiernan Monaco is a highly skilled and compassionate Doctor of Physical Therapy dedicated to helping individuals restore movement, reduce pain, and return to the activities they love. Known for her patient-centered approach and commitment to clinical excellence, she combines evidence-based treatment with genuine care and empathy.
Dr. Kiernan Monaco is a highly skilled and compassionate Doctor of Physical Therapy dedicated to helping individuals restore movement, reduce pain, and return to the activities they love. Known for her patient-centered approach and commitment to clinical excellence, she combines evidence-based treatment with genuine care and empathy.
A proud Long Island, NY native, Dr. Monaco earned her Bachelor of Science in Exercise Science with a Minor in Strength and Conditioning from the University of Delaware. During her undergraduate years, she developed a strong foundation in human movement and injury prevention, while also working as a certified cycle instructor, blending her love for fitness and teaching.
Her passion for physical therapy expanded globally when she traveled to New Zealand to study the international impact of the profession. She later earned her Doctorate in Physical Therapy from Long Island University in Brooklyn, where she continued to grow as a clinician and advocate for holistic, functional rehabilitation.
 Dr. Monaco is deeply committed to lifelong learning and advancing rehabilitation care. She participated in a global health service trip to Ghana, where she provided hands-on therapy for children with special needs and gained invaluable insight into community-based care. Her interest in innovative treatment approaches also led her to conduct research on virtual reality in pediatric physical therapy, which was accepted for presentation at the APTA New York 2025 Conference.
Dr. Monaco is deeply committed to lifelong learning and advancing rehabilitation care. She participated in a global health service trip to Ghana, where she provided hands-on therapy for children with special needs and gained invaluable insight into community-based care. Her interest in innovative treatment approaches also led her to conduct research on virtual reality in pediatric physical therapy, which was accepted for presentation at the APTA New York 2025 Conference.
Her treatment philosophy is rooted in treating the whole person, not just the injury. Kiernan focuses on long-term wellness, functional movement, and empowering patients to take an active role in their recovery and health journey
To schedule an appointment with Dr. Kiernan Monaco, call or email ActiveCare Physical Therapy today.
ActiveCare Physical Therapy™
29 West 38th Street, Suite 601
New York, NY 10018
Phone: (212) 777-4374
Email: staff@bestptnyc.com
Website: https://activecarephysicaltherapy.com
TMJ Disorders in NYC: How Physical Therapy Can Relieve Jaw Pain and Dysfunction
TMJ Disorders in NYC is an important topic for many patients experiencing jaw pain, headaches, and facial tension, and physical therapy can play a major role in treating these symptoms effectively.
Starting physical therapy can be both exciting and nerve-wracking—especially if it’s your first time. Whether you’re recovering from surgery, managing chronic pain, or trying to improve mobility, understanding what to expect during your first physical therapy session can help you feel more prepared and confident.
In this post, we’ll walk you through what typically happens at your first visit, including the evaluation process, common questions your therapist might ask, and how to dress and prepare. At ActiveCare Physical Therapy™ in New York City, our goal is to make your journey toward recovery clear, comfortable, and successful from day one.
Initial Evaluation: Laying the Foundation
Your first physical therapy session will primarily consist of a comprehensive evaluation. This is a critical step where your therapist gathers information to create a customized treatment plan tailored to your goals and needs.
Medical History Review
Expect your therapist to ask about:
- Your current condition or injury—when it started, what aggravates or relieves it
- Your medical history, including surgeries, past injuries, and chronic conditions
- Medications you are taking
- Your lifestyle, job, daily activities, and fitness level
All of this helps your therapist understand how your issue fits into the bigger picture of your health and movement patterns.
Physical Assessment
Once your history is discussed, your therapist will perform a detailed physical assessment that may include:
- Posture and gait analysis: to observe your natural stance and walking mechanics
- Range of motion testing: measuring how well your joints move
- Strength testing: assessing muscle power and endurance
- Palpation: hands-on techniques to feel muscle tension, swelling, or tenderness
- Functional movement screening: observing movements like squatting, bending, or reaching
These tests help identify the root cause of pain or dysfunction—not just where it hurts, but why it hurts.
Discussion of Findings and Goals
After your assessment, your physical therapist will explain their findings in a clear, easy-to-understand way. They will discuss:
- The suspected diagnosis or contributing factors to your symptoms
- Short- and long-term goals for your therapy
- A general outline of your treatment plan
This is also a great time to ask any questions you have about your condition or the therapy process.
First Treatment Begins
In many cases, treatment will begin during your first session. Depending on your condition, this may include:
- Gentle manual therapy or soft tissue work
- Light therapeutic exercises
- Postural or movement corrections
- Modalities such as heat, ice, or electrical stimulation (if appropriate)
The goal is to start you on the path to healing without overwhelming your system. Your therapist will also provide home exercises to reinforce what you learned during the session.
How to Prepare for Your First Visit
To make the most of your session:
- Wear comfortable clothing: Choose attire that allows movement and easy access to the area being treated.
- Arrive early: Give yourself time to complete paperwork and relax before your appointment.
- Bring relevant documents: Include prescriptions, imaging reports, and insurance info.
- Come with questions: Jot down anything you’re curious or concerned about—it’s your time to learn!
What Happens Next?
At the end of your session, your therapist will recommend a frequency for follow-up visits (typically 1–3 times per week) and may give you exercises to do at home. The consistency of your therapy—both in the clinic and at home—plays a major role in how quickly and effectively you recover.
TMJ Disorders in NYC: Conclusion
Your first physical therapy session is all about assessment, education, and beginning a personalized plan to help you heal. At ActiveCare Physical Therapy™, we prioritize one-on-one care to ensure your treatment is tailored to your body, goals, and lifestyle. By understanding what to expect, you’ll feel more confident and empowered as you begin your recovery journey.
ActiveCare Physical Therapy
29 West 38th Street
Suite 601
New York, NY 10018
(212) 777-4374
Move Well This Thanksgiving
The 2025 Thanksgiving season brings travel, cooking, and celebration, and all of it can place extra stress on your body. At ActiveCare Physical Therapy, we want you to enjoy the holiday without discomfort.
Dr. Karena Wu, Clinical Director and Owner, reminds us: “The body thrives on movement. Even a few minutes of activity during busy holidays can prevent stiffness and keep you feeling your best.”
Quick tips for a healthier Thanksgiving:
- Take movement breaks: Stand, stretch, or walk every hour during long travel or long meals.
- Balance big meals with a short walk: A brief walk can support digestion and reduce stiffness.
- Protect your back in the kitchen: Shift your weight, keep essentials within easy reach, and stretch when you can.
- Stay hydrated: Water helps your muscles stay flexible.
If discomfort or pain lingers, the team at ActiveCare Physical Therapy is ready to help you feel better and move better this season.
Contact us at 212-777-4374 to schedule your next session and start the holidays feeling your best.
Wishing you a healthy and comfortable Thanksgiving from the team at ActiveCare Physical Therapy!
How ActiveCare Physical Therapy Uses Advanced Techniques for Recovery
 ActiveCare Physical Therapy, led by Karena Wu PT in New York City, is known for blending expert clinical care with innovative techniques to accelerate recovery, reduce pain, and enhance mobility. As a Board-Certified Clinical Specialist in Orthopedic Physical Therapy, Karena Wu and her team leverage the latest in manual therapy, movement science, and technology to deliver customized rehabilitation solutions.
ActiveCare Physical Therapy, led by Karena Wu PT in New York City, is known for blending expert clinical care with innovative techniques to accelerate recovery, reduce pain, and enhance mobility. As a Board-Certified Clinical Specialist in Orthopedic Physical Therapy, Karena Wu and her team leverage the latest in manual therapy, movement science, and technology to deliver customized rehabilitation solutions.
In this article, we explore the advanced techniques ActiveCare Physical Therapy™ uses to ensure patients receive world-class care, whether recovering from injury, managing chronic conditions, or improving performance.
1. Orthopedic Manual Therapy
At the core of ActiveCare’s approach is advanced manual therapy. Karena Wu is fellowship-trained through the American Academy of Orthopaedic Manual Physical Therapists (AAOMPT), a prestigious credential that reflects rigorous training in joint mobilization, soft tissue techniques, and clinical reasoning.
This allows the team to:
- Quickly identify biomechanical dysfunctions
- Target the root cause of pain—not just the symptoms
- Use hands-on techniques to restore motion and reduce inflammation
Manual therapy is often combined with corrective exercise to ensure long-term relief and functional improvement.
2. Pilates-Based Rehabilitation
ActiveCare integrates Pilates into physical therapy to strengthen core musculature, improve body awareness, and support spine health. This approach is ideal for treating conditions like:
- Low back pain
- Pelvic instability
- Postural imbalances
- Post-operative rehabilitation
Patients benefit from individualized Pilates sessions that focus on form, breath control, and controlled resistance—often using equipment such as the Reformer or Cadillac.
3. Neuromuscular Re-Education
A key component of recovery involves retraining the brain-body connection. The therapists at ActiveCare use neuromuscular re-education to correct faulty movement patterns and enhance muscle coordination.
This technique is especially beneficial for patients with:
• Chronic pain
• Muscle imbalances (such as Upper Cross Syndrome)
• Post-stroke deficits
• Sports-related movement dysfunctions
Through targeted cueing and progressive exercises, patients learn to move efficiently and reduce compensatory habits that can lead to further injury.
4. Myofascial Decompression (Cupping)
ActiveCare utilizes myofascial decompression, or cupping therapy, as part of soft tissue treatment. Unlike traditional massage, this technique lifts the tissue away from the body using negative pressure, helping to:
- Reduce muscle adhesions
- Improve circulation
- Increase tissue hydration and glide
Cupping is commonly used in conjunction with active movement and stretching to maximize results.
5. Kinesiology Taping
Kinesiology tape is applied to support joints and muscles while still allowing for full range of motion. At ActiveCare, taping is customized based on the patient’s needs—whether it’s unloading a tendon, reducing swelling, or promoting postural awareness.
6. Fit3D Body Scanning for Baseline & Progress Tracking
To precisely measure changes in body composition, posture, and alignment, ActiveCare uses the Fit3D Body Scanner. This technology captures a 360° view of the body, offering:
- Objective postural assessments
- Accurate tracking of muscle mass, symmetry, and weight distribution
- Baseline data to guide treatment goals
Patients receive progress reports that visually reinforce their improvements, boosting motivation and compliance.
7. Acupuncture & Dry Needling
When appropriate, ActiveCare offers acupuncture and dry needling to reduce muscle tension, improve blood flow, and stimulate healing. These techniques are particularly effective for:
• Trigger points
• Sciatica
• Joint stiffness
• Chronic inflammation
8. Telehealth & Hybrid Care Options
ActiveCare Physical Therapy™ also offers telehealth sessions for patients who need virtual access to care. These sessions include guided exercises, postural assessments, ergonomic advice, and progression of home programs. For many patients, telehealth serves as an excellent complement to in-person visits.
ActiveCare Physical Therapy™ Advanced Techniques for Recovery: Conclusion
At ActiveCare Physical Therapy™, advanced recovery isn’t just about what tools are used—it’s about how they’re used, when they’re applied, and how well they are tailored to each individual. The combination of evidence-based manual therapy, Pilates, movement science, and cutting-edge technology ensures that every patient receives the most effective and efficient path to recovery.
Get Started with Expert Care
Whether you’re dealing with post-surgical recovery, sports injuries, or chronic pain, the team at ActiveCare Physical Therapy™ is ready to help you heal better, faster, and with long-term results.
ActiveCare Physical Therapy™
29 West 38th Street, Suite 601
New York, NY 10018
Phone: (212) 777-4374
Email: staff@bestptnyc.com
Website: https://activecarephysicaltherapy.com
Recover Faster After the NYC Marathon — Free 15-Minute Recovery Sessions at ActiveCare PT by Bryant Park!
Just crossed the NYC Marathon finish line? Congratulations! You’ve put your body through an incredible test of endurance; now it’s time to give it the recovery it deserves. Join us at ActiveCare Physical Therapy by Bryant Park for a FREE 15-minute Recovery Session designed to help marathon runners bounce back faster and feel their best.

All you need to do is bring your finisher’s medal to gain exclusive access to our intermittent compression boots, which help reduce muscle soreness, improve circulation, and speed up recovery. These complimentary sessions will be available for three days following the NYC Marathon, but spots are limited so don’t wait to secure yours!
👉 Give us a call at 212-777-4374 to reserve your spot today.
Take Your Performance to the Next Level with a Fit3D Body Scan
While you’re here, experience our Fit3D body scan, a cutting-edge assessment tool that provides a 360° view of your body composition and posture. For athletes and marathon runners, the Fit3D scan delivers invaluable insights — tracking muscle balance, identifying asymmetries, and monitoring changes in body composition over time. This data helps optimize your training, prevent injury, and measure progress beyond what the scale can show.
Recovery and performance go hand in hand, and at ActiveCare PT, we’re here to support both every step of the way.

ActiveCare Physical Therapy™
29 West 38th Street, Suite 601
New York, NY 10018
Phone: (212) 777-4374
Email: staff@bestptnyc.com
Website: https://activecarephysicaltherapy.com
October is National Physical Therapy Month: Hip Health
At ActiveCare Physical Therapy, we are celebrating by focusing on hip health for everyone from athletes to non-athletes and all ages. Whether you are running a marathon, walking your dog, or simply getting in and out of a chair, your hips play a vital role in everyday movement.
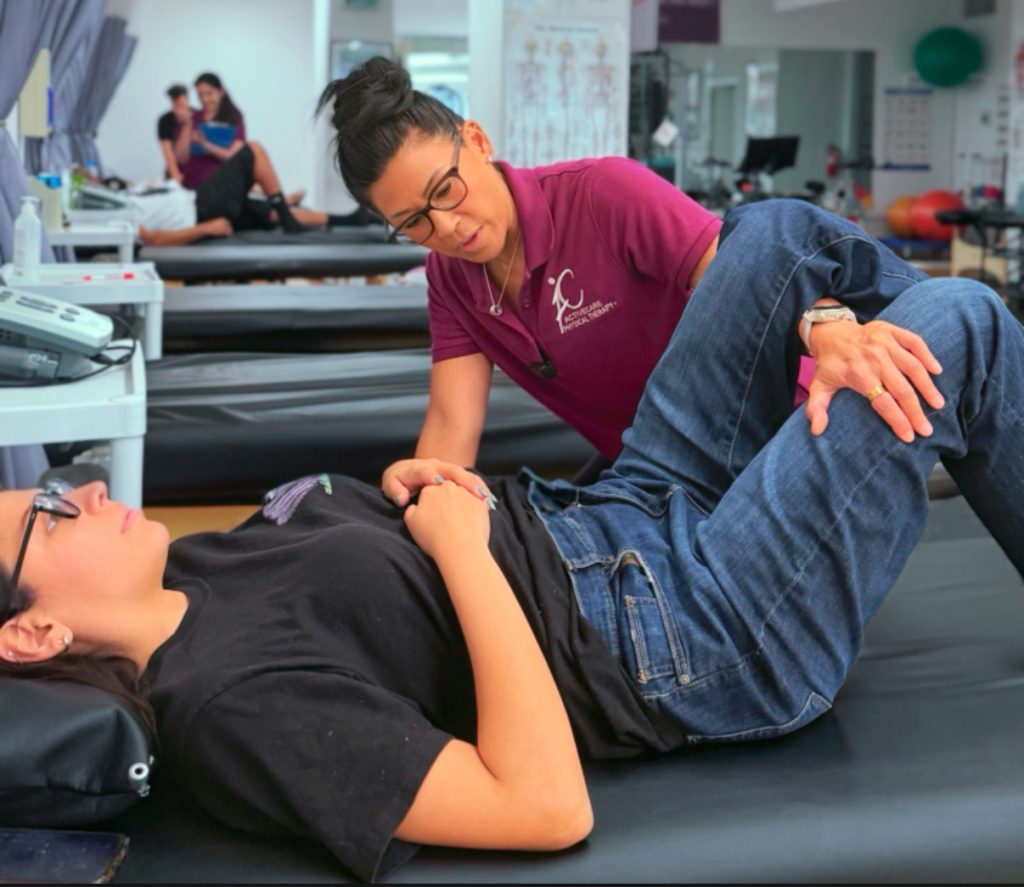
Did you know hip pain and stiffness can limit mobility, affect performance, and lower your quality of life? Physical therapy can help. At ActiveCare PT, we specialize in manual therapy along with targeted exercises to relieve pain, improve strength, and restore function so you can move with ease and confidence.
Dr. Karena Wu, Owner and Clinical Director of ActiveCare PT, says “The hips are the foundation for so much of what we do. Maintaining strength and mobility is key to staying pain free and enjoying life.”
This National PT Month, take the first step toward better hip health. Contact ActiveCare Physical Therapy today to schedule your consultation.
ActiveCare Physical Therapy™
29 West 38th Street, Suite 601
New York, NY 10018
Phone: (212) 777-4374
Email: staff@bestptnyc.com
Website: https://activecarephysicaltherapy.com
The Importance of Manual Therapy in Treating Injuries
When it comes to recovering from injury, managing chronic pain, or improving mobility, manual therapy stands out as a cornerstone of effective physical rehabilitation. At ActiveCare Physical Therapy™ in New York City, led by Karena Wu PT, a Board-Certified Clinical Specialist in Orthopedic Physical Therapy, manual therapy is not just an add-on—it’s a primary treatment strategy that accelerates healing, restores function, and reduces pain.
In this post, we’ll explore what manual therapy is, why it’s essential in treating injuries, the different techniques involved, and how it fits into a comprehensive physical therapy plan.

What Is Manual Therapy?
Manual therapy refers to hands-on techniques used by licensed physical therapists to assess and treat musculoskeletal pain and dysfunction. Unlike exercises or modalities like ultrasound or electrical stimulation, manual therapy involves direct contact with the patient’s body to improve tissue extensibility, mobilize joints, and reduce soft tissue restrictions.
Key Benefits of Manual Therapy
Manual therapy is highly effective for treating a wide range of conditions, including acute injuries, post-surgical rehabilitation, and chronic pain syndromes. Its primary benefits include:
- Pain relief: Mobilization of joints and soft tissues reduces mechanical stress and stimulates the nervous system to inhibit pain signals.
- Improved mobility: Manual therapy can help restore normal range of motion in joints and surrounding muscles.
- Enhanced circulation: Increased blood flow to the affected area supports tissue healing and reduces inflammation.
- Faster recovery: By breaking down scar tissue and improving movement quality, manual therapy expedites healing.
Common Manual Therapy Techniques
1. Joint Mobilization
This technique involves the passive movement of joints using controlled oscillations or sustained holds. It’s especially helpful in relieving stiffness in the spine, shoulders, hips, and knees.
2. Soft Tissue Mobilization (STM)
Soft tissue techniques are used to break down adhesions, improve tissue flexibility, and reduce muscle spasms. This may include deep tissue massage, myofascial release, and trigger point therapy.
3. Myofascial Release
This gentle yet targeted method releases restrictions in the fascia—the connective tissue that surrounds muscles and organs. It’s particularly beneficial for individuals with chronic pain or postural dysfunction.
4. Manual Stretching
A therapist-guided stretch can be more effective and safer than stretching alone. Manual stretching is often used to increase flexibility and relieve tightness in injured areas.
5. Muscle Energy Techniques (MET)
These involve the patient actively contracting muscles in a specific direction while the therapist resists. MET can realign joints, reduce muscle tightness, and improve movement.
Who Should Receive Manual Therapy?
Manual therapy is appropriate for a wide range of injuries and conditions, including:
- Low back pain and sciatica
- Neck pain and whiplash
- Shoulder impingement and frozen shoulder
- Hip and knee osteoarthritis
- Post-surgical joint stiffness
- Sports injuries like strains, sprains, and overuse syndromes
Your physical therapist will determine which techniques are best suited for your specific condition and goals.
Manual Therapy + Exercise = Optimal Results
Manual therapy is not a stand-alone solution—it’s most effective when combined with therapeutic exercise and movement re-education. Hands-on treatment helps restore mobility and relieve pain, while exercise builds strength, coordination, and long-term resilience.
At ActiveCare Physical Therapy™, manual therapy is integrated into a full-spectrum rehabilitation approach. Patients benefit from expert hands-on care followed by individualized corrective exercise programs to ensure lasting results.
Conclusion
Manual therapy plays a vital role in physical therapy by accelerating healing, improving function, and reducing pain. Its effectiveness lies in the therapist’s hands-on ability to diagnose, treat, and improve movement at a deep and targeted level.
If you’re experiencing pain, recovering from an injury, or simply want to move better, manual therapy could be the game-changer in your recovery journey.
Contact Information
ActiveCare Physical Therapy™
29 West 38th Street, Suite 601
New York, NY 10018
Phone: (212) 777-4374
Email: staff@bestptnyc.com
Website: https://activecarephysicaltherapy.com
 ActiveCare Physical Therapy, PC
ActiveCare Physical Therapy, PC
29 West 38th Street
Suite 601
New York, NY 10018

